Healthcare Analytics Series: Enrollment Data for Health Insurance Exchange (HIX) Plans
With the open enrollment period (OEP) on HealthCare.gov set to start on November 1, 2022, we thought it would be a good time to review health insurance exchange (HIX) plans with a focus on policy and enrollment trends.
The 2010 Affordable Care Act (ACA) gave rise to the Health Insurance Marketplace, or health insurance exchange (HIX), which allows individuals and small businesses to apply for and enroll in private health insurance (commercial) plans. Health insurance policies offered through the HIX are qualified health plans (QHPs), which means the coverage includes essential health benefits and meets affordability requirements within the ACA. According to data from the Centers for Medicare & Medicaid Services (CMS) OEP Snapshot Reports, the number of individuals enrolled in HIX plans held fairly steady from 2017 to 2021. During that time, the annual value never differed from the mean (11.8 million) by more than 4%.
However, in 2022, the number of HIX plan enrollees increased by more than 20%, according to a press release from the Department of Health and Human Services (HHS), with enrollment likely driven higher by disruptions in employer-sponsored insurance (ESI) in response to the pandemic’s impact on employment and a range of enhanced financial support for HIX enrollees contained in the American Rescue Plan Act (ARPA). The ARPA not only included enhanced premium tax credits (ePTCs), but also removed the upper limit on household income to qualify for an 8.5% limit on the amount of income spent on health insurance premiums. When combined with existing financial support for HIX plans, the overall effect was to drive enrollment in such plans to a record-setting level in 2022 (14.5 million).
The enhanced financial support for HIX plans in the ARPA was originally set to expire at the end of fiscal year (FY) 2022, but the Inflation Reduction Act of 2022 (IRA) extended the main financial support. This support—ePTCs and the removal of income caps for the household premium cap—are now law until the end of FY 2025. With these measures in place, enrollment in HIX plans is likely to grow even more due to the increased affordability of plans.
HIX plan enrollment will also likely rise in coming years due to other policy-related actions, such as the Biden administration’s announced fix for the “family glitch” and the eventual termination of the COVID-19 public health emergency (PHE). On the last point, Congress provided a financial incentive to states in the early days of the pandemic through a 6.2% enhanced payment for the federal portion of Medicaid spending, so long as states suspended redetermination, the once-annual process of re-establishing eligibility for Medicaid recipients. This pause in redetermination is tied to a PHE first effective in January 2020, which has been extended every 90 days by the Secretary of HHS. According to the most recent data from CMS covering the period from February 2020 to June 2022, combined enrollment in Medicaid and the State Children's Health Insurance Program (CHIP) has increased by more than 18.5 million during the pandemic, a jump of more than 25%.
However, with COVID-19 vaccinations widely available and case counts on the decline in the U.S. in 2022, an end to the PHE is increasingly likely. In preparation, CMS has been conducting a series of monthly webinars with stakeholders to discuss the Medicaid “unwinding” process, which will take place once redetermination restarts. Central to CMS’s unwinding message is the importance of continuity of coverage, i.e., helping eligible individuals transition seamlessly from Medicaid to another form of health insurance. Furthermore, HIX plans are expected to be the new form of coverage for many of those deemed ineligible for Medicaid, i.e., for individuals redetermined out of Medicaid.
Although a single marketplace is mentioned above, the ACA actually gave rise to a collection of marketplaces. The federal website, HealthCare.gov, serves as a central starting point for consumer inquiries about HIX plans, but HIX enrollment and operations are sometimes handled by individual states, which operate separate state-based exchanges (SBEs). In 2022, the majority of states still rely on HealthCare.gov, the federally facilitated exchange (FFE) platform, for enrollment services.
Tableau-Based HIX Plan Enrollment Dashboard Developed by Forte Analytics
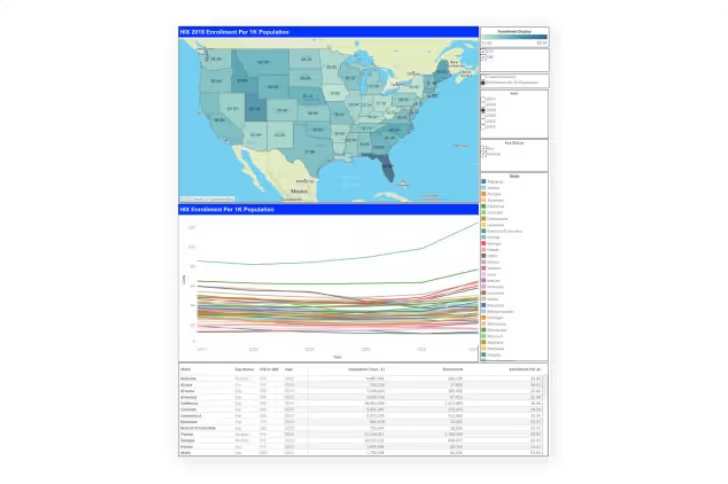
Forte Analytics developed a business intelligence tool in Tableau using HIX plan enrollment data for plan years 2017–2022, as published by CMS. The tool features a dashboard that allows the user to filter by several options, including: 1) exchange type (FFE or SBE); 2) plan year; and 3) each state’s Medicaid expansion status. In addition, the data can be displayed as raw counts of enrollees or as enrollment per 1,000 population. (Population data reflect the U.S. Census Bureau’s estimate of each state’s population in the year before the plan year, e.g., the 2019 population estimates are used to normalize the 2020 plan year enrollment data.)
Hovering over a state brings the state’s HIX enrollment data into focus in the line graph shown. The raw counts reveal that enrollment grew for nearly all states from 2021 to 2022, with enrollment decreasing in only three states (Hawaii, Kentucky, and Massachusetts) and Washington, D.C. During that period, Florida grew the most by raw count (602,744), while Texas grew the most by percentage (nearly 30%). Both are Medicaid non-expansion states.
The normalized data highlight the important role of HIX plans in Medicaid non-expansion states, as the rate of enrollment in HIX plans in 2022 for non-expansion states (57.0 per 1,000) was more than 75% greater than the rate of HIX plan enrollment for expansion states (32.3 per 1,000). Moreover, seven of the top 10 states ranked by normalized HIX plan enrollment for the same year are Medicaid non-expansion states. The importance of HIX plans to individuals and families with lower incomes is also evident in demographic data on enrollees (not shown), which tend to show disproportionately high levels of enrollment for the population with lower incomes (100–200% of federal poverty level) relative to the state’s overall population. This finding is especially true for Medicaid non-expansion states. (Contact us for details of the analysis.)
This business intelligence tool provides a range of insights tailored to support decision-making and analysis related to this small but growing component of the commercial line of health insurance business. Forte Analytics has also built a Tableau-based tool to review HIX plan quality ratings by plan type and group affiliation (quality metrics tool not shown). The data for the second tool come from the performance system CMS developed for HIX plans known as the Quality Rating System (QRS).
What do you think of our approach? Have you used other methods or tools to analyze these complex data? We would love to hear your thoughts and comments on this topic.
Over the coming weeks, we will be posting more features in this series. Future subjects will include additional business intelligence tools, as well as artificial intelligence/machine learning (AI/ML) techniques Forte Analytics uses in risk assessment, forecasting, and correlation, among other objectives. The articles will focus on projects and tools using public data sources to avoid any restrictions associated with commercially available data sets, e.g., commercial claims data that we also rely upon in our daily work for clients.
Thanks for reading and please reach out if you have any questions or would like to have a follow-up discussion.
Forte Analytics provides analysis and business intelligence to major players across the health care landscape.
By Darren Michael and Molly Maskrey
With technical support and feedback provided by John Wendel, Conor Frye, Sam Moore, Ed McCauley, and Diana Hodges